The Impact of Reprocessing Downtime in Gastroenterology Department
In the realm of medical technology, automated systems have revolutionized various facets of healthcare, including the gastrointestinal (GI) department. Automated flushing systems have emerged as a game-changer in GI departments, offering an array of benefits that streamline processes and enhance patient care. These advantages, which include increased productivity, the elimination of manual syringe flushing, and improved compliance, have significantly transformed the landscape. However, as with any technology, there are potential pitfalls, particularly when these automated flushing systems experience downtime.
Advantages of Automated Flushing Systems in GI Departments
Before diving into the challenges associated with downtime of automated flushing systems, let’s explore the key advantages that have made them indispensable tools in GI departments:
- Enhanced Productivity: Automated flushing systems have redefined efficiency in GI departments by optimizing workflow. These systems can flush multiple lumens at once, slashing processing time and allowing medical
 staff to redirect their time and energy towards other critical tasks.
staff to redirect their time and energy towards other critical tasks. - Elimination of Manual Flushing: Traditionally, healthcare professionals were tasked with manually flushing medical equipment using syringes. This repetitive motion not only consumed valuable time but also increased the risk of repetitive strain injuries. Automated systems have eradicated the need for manual flushing, promoting the well-being of nurses and technicians and reducing the likelihood of workplace-related injuries.
- Elevated Compliance: Automated flushing systems ensure uniformity in reprocessing, enhancing compliance with SOP’s and regulations. This consistency enables nurses to trust that devices are being cleaned to standards, translating to ensured patient safety and adherence to regulatory standards.
Challenges When Automated Flushing Systems Experience Downtime
As advanced as automated flushing systems are, some are more reliable than others. The repercussions of flushing system downtime in GI departments can be profound and wide-reaching:
- Workflow Disruption: A sudden breakdown in an automated flushing system can disrupt the meticulously planned workflow of a GI department. Processes that rely on the system’s efficiency may be delayed, potentially leading to prolonged turnaround times and a decrease in overall departmental productivity.
- Return to Manual Labor: In the absence of functioning automated systems, nurses and technicians may have to revert to manual flushing methods such as using syringes. This not only prolongs the scope reprocessing
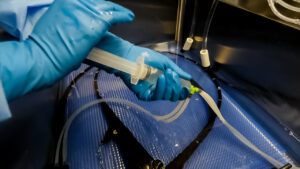 time, but also reintroduces the risk of repetitive strain injuries.
time, but also reintroduces the risk of repetitive strain injuries. - Compliance Vulnerability: Standardized processes can be compromised when automated systems are out of commission. Nurses and technicians may need to improvise or revert to old methods, leading to deviations from established procedures that could compromise patient safety and IFU compliance.
- Resource Allocation: When automated systems fail, departments may need to allocate additional resources, including personnel and time, to fix problems. This reallocation of resources is an unnecessary pain, and leads to other costs such as overtime.
- Patient Care Impact: All these negative consequences compound and compromise patient safety, the ultimate promise made by all technicians and nurses.
Conclusion
Automated flushing systems have revolutionized the way GI departments operate, offering a range of benefits that optimize processes and enhance patient care. However, downtime associated with unreliable automated flushing solutions can create more headaches than GI nurses bargained for.
Interested in more GI blog posts on The Reprocessing Report? Click here to dive in!