In a recent Reprocessing Report post, we explored why and how copper has found its way into our hospitals. Copper’s organic ability to denature and kill, its cost effectiveness relative to other anti-bacterial solutions, and active, continuous process of killing pathogens provides compelling rationale for copper to supplement existing infection control practices.
The Centers for Health Design 2015 Study1
Reduction of Hospital Acquired Infections (HAIs)
In a study performed by the Copper Development Association, Faculty of Natural and Environmental Sciences, and Medical University of South Carolina, copper-alloy surfaces were tested for their ability to kill various bacteria on high-touch surfaces. This was done in both laboratory and in hospital patient room settings. The study

further sought to understand if copper could reduce HAIs in the rooms in which it was used.
The study tested numerous bacteria against copper-alloy surfaces: methicillin-resistant staphylococcus aureus (MRSA), vancomycin-resistant enterococci (VRE), Escherichia coli (E.coli), clostridium difficile (C. difficile), influenza A, and norovirus.
The study found that the copper was able to reduce live bacteria on its surfaces by over 99.9% in laboratory testing. When testing copper for its ability to self-sanitize under wet and dry conditions, copper retained over a 99.9% reduction over the course of 84 tests.
A further demonstration to test if copper continued to perform over long periods of time, copper had over a 99.9% reduction in bacteria in 72 of 84 tests when determining its ability to provide continuous reduction of bacteria on its surface.
The clinical trial, conducted in the intensive care units (ICUs) of Memorial Sloan Ketting Cancer Center, Medical University of South Carolina, and Ralph H. Johnson Veterans Administration Medical Center, aimed to duplicate these findings in the patient room. Areas such as bed rails, call buttons, tray tables, and IV poles were installed with copper-alloy components. In Phase 2 of the trial, weekly samples of bacteria were taken from rooms installed with the copper-alloy components, and those without. Over 21 months, the average reduction in microbial burden on copper-alloy components was 83% greater than non-copper surfaces.
The study wanted to go one step further: could copper be linked to a reduction in HAIs? The study noted that a copper-alloy application on 10% of high-touch surfaces can contribute to a 58% reduction of patient infections, demonstrating its high impact.
The 2015 study provides a couple provoking ideas:
- Copper is successful in reducing microbial load against a wide range of bacteria in clinical settings.
- Even in small doses, copper can significantly reduce microbial load. Targeted application can provide significant results.
- Copper surfaces work to self-sanitize in a range of conditions, from wet to dry. Unlike other metals, copper’s anti-microbial properties did not lessen over the course of time.
- Copper requires no change in human behavior to be effective, making implementation simple, and seamless relative to other disinfection procedures.
American Society for Microbiology (ASM) 2019 Study2
An additional study, published by the American Society of Microbiology, sought to replicate the impressive results seen in the patient room. In a study between control patient beds, mostly made of plastic, and interventional beds made of almost entirely copper-alloy surfaces, routine samples were taken of bacteria on various surface points and tested for contamination.
The study similarly found shocking results: the average microbial burden on the copper-alloy surface beds was 94% less than that of the plastic control beds. The study further found that over the course of the 11-month testing period, the copper-alloy surfaces maintained their bactericidal effectiveness. Daily cleaning with quaternary ammonium-based disinfectants did not impact the outcome of the copper-alloy surface’s anti-microbial properties.
Implications for Practice
Both studies found sustained, active results of reduced microbial load after deploying copper-alloy in high-touch environments. Further, both studies demonstrated surface disinfection practices didn’t have to be changed for copper to positively impact disinfection outcomes.
In its discussion points, the 2019 ASM study states, “The Joint Commission infection control standard (IC) 02.02.01 presently requires hospitals to reduce the risk of infections associated with medical equipment, devices, and supplies.2,3”
While more data could be provided to substantiate copper’s impact in other areas of the hospital, and copper’s role in fulfilling this TJC standard, the outlook is positive. It is exciting that a problem as pervasive as HAIs may be battled with a tool we’ve long understood and used. Not all challenges require complex innovations to solve.
Looking to see how copper can be implemented in another high-touch area of your department: your decontamination sink? Contact us to learn how Pure Processing is integrating the newest (and yet age-old tested!) technologies into our sterile processing & endoscopy spaces to reduce HAIs.
Work Cited
- Michels, H. T., Keevil, C. W., Salgado, C. D., & Schmidt, M. G. (2015, July 10). From laboratory research to a clinical trial: Copper alloy surfaces kill bacteria and reduce hospital-acquired infections. National Library of Medicine. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4561453/
- Schmidt, M. G., Attaway, H. H., Fairey, S. E., Howard, J., Mohr, D., & Craig, S. G. (2019). Self-Disinfecting Copper Beds Sustain Terminal Cleaning and Disinfection Effects throughout Patient Care. Applied and Environmental Microbiology, 86(1). https://doi.org/10.1128/aem.01886-19
- The Joint Commission. 5 September 2018. Accreditation and certification—4-1-1 on survey enhancements: new scoring revisions for IC.02.02.01 now in effect. The Joint Commission Online, Oak Brook, IL.


 daunting. The two simple questions asked above hold the potential to become the catalyst for workgroups and committees of stakeholders that can come together to address the problem(s) you’re facing. That problem we all want fixed, we quickly realize is not such an easy fix, after all. Hours of research, planning and implementation are now committed to the process improvement plan set forth.
daunting. The two simple questions asked above hold the potential to become the catalyst for workgroups and committees of stakeholders that can come together to address the problem(s) you’re facing. That problem we all want fixed, we quickly realize is not such an easy fix, after all. Hours of research, planning and implementation are now committed to the process improvement plan set forth.


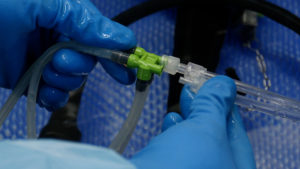
 endoscopes. Automated flushing systems make flushing scopes much easier, while eliminating a painful repetitive motion that has the potential to lead to carpal tunnel complaints.
endoscopes. Automated flushing systems make flushing scopes much easier, while eliminating a painful repetitive motion that has the potential to lead to carpal tunnel complaints.



 their set up to ensure compliance.
their set up to ensure compliance.






